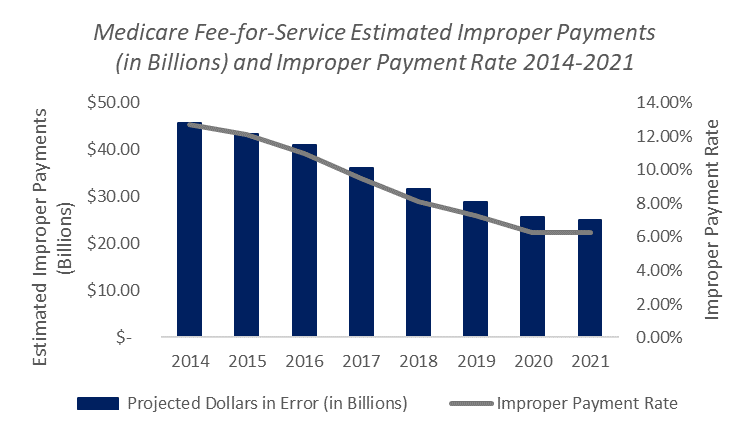
The Centers for Medicare & Medicaid Services (CMS) announced today that CMS’ aggressive corrective actions led to an estimated $20.72 billion reduction of Medicare Fee-for-Service (FFS) improper payments over seven years.
“CMS is undertaking a concerted effort to address the root causes of improper payments in our programs,” said CMS Administrator Chiquita Brooks-LaSure. “The continued reduction in Medicare fee-for-service improper payments represents considerable progress toward the Biden-Harris Administration’s goal of protecting CMS programs’ sustainability for future generations. We intend to build on this success and take the lessons we’ve learned to ensure a high-level of integrity across all of our programs.”
Improper payments are payments that do not meet CMS program requirements. Improper payments can be overpayments or underpayments, or payments where insufficient information was provided to determine whether a payment is proper or not. Most improper payments involve situations where a state or provider missed an administrative step. While fraud and abuse may lead to improper payments, it is important to note that the vast majority of improper payments do not constitute fraud, and improper payment estimates are not fraud rate estimates.
“CMS is committed to reducing and preventing improper payments,” said Jonathan Blum, CMS Principal Deputy Administrator & Chief Operating Officer. “It is important to understand that only a small fraction of improper payments represent a payment that should not have been made – and an even smaller percentage represent actual cases of fraud.”
The 2021 Medicare FFS estimated improper payment rate (claims processed July 1, 2019 to June 30, 2020) is 6.26% ̶ an historic low. This is the fifth consecutive year the Medicare FFS improper payment rate has been below the 10% threshold for compliance established in the Payment Integrity Information Act of 2019. Due to CMS corrective actions, the agency saw key successes in the following areas:
- Inpatient Rehabilitation Facility claims had a $1.81 billion decrease in estimated improper payments from 2018 to 2021. This is the result of years of sustained effort from CMS, which included clarifying policy to reduce provider burden and educating providers through the Targeted Probe and Educate program. CMS uses the Targeted Probe and Educate program to provide one-on-one help to providers, focusing on those who have high denial rates or unusual billing practices, to reduce claim errors and denials.
- Durable Medical Equipment (DME) claims saw a $388 million reduction in estimated improper payments since 2020 due to a nationwide expansion of prior authorization of certain DME items as well as the Targeted Probe and Educate program.
The FY 2021 Part C improper payment estimate reported is 10.28%. The 2021 Part C error rate estimate is not comparable to prior years because CMS refined the error rate calculation methodology.
The FY 2021 projected Part D improper payment rate is 1.58%. The slight increase is likely due to year-over-year variability.
CMS Completes PERM’s New Eligibility Reviews for Medicaid and CHIP
The Payment Error Rate Measurements (PERM) program uses a 17-states-per-year, 3-year rotation to identify and measure improper payments in Medicaid and the Children’s Health Insurance Program (CHIP). These include payments where a small administrative step was missed – such as after documentation was verified, it was not properly saved. All 50 states and the District of Columbia are reflected in the national Medicaid and CHIP improper payment rates reported, as that rate includes findings from the most recent 3 years of measurements (2019, 2020, and 2021). This year’s PERM results show that the 2021 Medicaid improper payment rate was 21.69%, and the CHIP improper payment rate was 31.84%. In the 2021 national Medicaid rate, 88% of improper payments were due to insufficient documentation. The majority of insufficient documentation errors represent situations where the required verification of eligibility data, such as income, was not appropriately documented.
“CMS is taking an agency-wide approach to addressing improperly documented payments,” said Dan Tsai, Deputy Administrator and Director, Center for Medicaid and CHIP Services. “CMS is committed to lowering the improper payments rate by focusing on documentation and information-sharing efforts. In Medicaid, that means working closely with states to implement best practices and ensure they maintain the proper documentation.”
CMS paused PERM eligibility reviews from 2015 to 2018, as states were implementing new rules under the Affordable Care Act for determining eligibility for many beneficiaries. During the pause of the PERM program’s eligibility measurement component, CMS required states to implement quality control pilots to ensure effective oversight and monitoring of Medicaid eligibility determinations while CMS revamped the PERM eligibility review component to accurately measure eligibility determination changes under the Affordable Care Act. CMS began utilizing an updated eligibility component beginning in the FY 2019 measurement cycle, so this year’s PERM measurement is the first year CMS has PERM data for all 50 states and the District of Columbia under the updated PERM eligibility review component. This gives CMS root cause analysis data to prioritize CMS’ efforts to focus on and minimize true improper payments and work with states to address inadequate documentation.
CMS has undertaken an effort to assess all improper payment programs to evaluate the best way to distinguish true improper payments from potentially proper payments, specifically focusing on errors due to inadequate documentation errors. In addition, CMS is evaluating the best approach to allow CMS and states to prioritize identification and compliance actions against instances that represent “true” improper payments to the program.
“We are committed to protecting our programs’ sustainability, and CMS’ work to reduce improper payments will continue to focus on developing and implementing policies to ensure payments are made correctly,” said Dara Corrigan, CMS Deputy Administrator and Director, Center for Program Integrity.
More information on the agency’s improper payments for Medicare, Medicaid, and CHIP can be found at https://www.cms.gov/ImproperPayments
To view a Fact Sheet on Improper Payments, visit https://www.cms.gov/newsroom/fact-sheets/improper-payments-fact-sheet
To view the HHS Agency Financial Report, visit: https://www.hhs.gov/about/agencies/asfr/finance/financial-policy-library/agency-financial-reports/index.html
###
Get CMS news at cms.gov/newsroom, sign up for CMS news via email and follow CMS on Twitter @CMSgov