At Risk: Pre-Existing Conditions Could Affect 1 in 2 Americans:
129 Million People Could Be Denied Affordable Coverage Without Health Reform
Introduction
According to a new analysis by the Department of Health and Human Services, 50 to 129 million (19 to 50 percent of) non-elderly Americans have some type of pre-existing health condition. Up to one in five non-elderly Americans with a pre-existing condition – 25 million individuals – is uninsured. Under the Affordable Care Act, starting in 2014, these Americans cannot be denied coverage, be charged significantly higher premiums, be subjected to an extended waiting period, or have their benefits curtailed by insurance companies.
As many as 82 million Americans with employer-based coverage have a pre-existing condition, ranging from life-threatening illnesses like cancer to chronic conditions like diabetes, asthma, or heart disease. Without the Affordable Care Act, such conditions limit the ability to obtain affordable health insurance if they become self-employed, take a job with a company that does not offer coverage, or experience a change in life circumstance, such as divorce, retirement, or moving to a different state. Older Americans between ages 55 and 64 are at particular risk: 48 to 86 percent of people in that age bracket have some type of pre-existing condition. And 15 to 30 percent of people in perfectly good health today are likely to develop a pre-existing condition over the next eight years, severely limiting their choices without the protections of the Affordable Care Act.
The last Congress passed and the President signed into law a new set of patient protections that prohibit insurance companies from denying coverage to Americans when they need it most. Starting in 2014, insurers can no longer carve out needed benefits, charge higher premiums, set lifetime limits on benefits, or deny coverage due to a person’s pre-existing condition. Individuals and small businesses will be able to purchase insurance through State-based Exchanges, competitive marketplaces for private health insurance. Tax credits will available for individuals and families with moderate incomes to ensure Exchange options are affordable for all.
A number of protections have already been put in place by the Affordable Care Act in 2010 and 2011 to increase access to health care coverage for those who need it. Insurers can no longer limit lifetime coverage to a fixed dollar amount or take away coverage because of a mistake on an application. Young adults have the option of staying as dependents on their parents’ coverage up to the age of 26 if they lack access to job-based insurance on their own, and insurers cannot deny coverage to a child because of a pre-existing condition. Thousands of uninsured people with pre-existing conditions have enrolled in the temporary high-risk pool program called the Pre-existing Condition Insurance Plan (PCIP), which has already saved people’s lives by covering services like chemotherapy.
All of these protections for Americans with pre-existing conditions would be taken away without the health reform law.
Pre-Existing Conditions as a Barrier to Health Care and Coverage
A “pre-existing condition” is a health condition that exists before someone applies for or enrolls in a new health insurance policy. Insurers generally define what constitutes a pre-existing condition. Some are obvious, like currently having heart disease or cancer. Others are less so – such has having asthma or high blood pressure. While insurers generally determine the presence of a pre-existing condition based on an applicant’s current health status, sometimes a healthy applicant can be deemed to have a pre-existing condition based on a past health problem or evidence of treatment for a particular condition.
Prior to the Affordable Care Act, in the vast majority of States, insurance companies in the individual and small group markets could deny coverage, charge higher premiums, and/or limit benefits to individuals based on pre-existing conditions. A recent national survey found that 36 percent of those who tried to purchase health insurance directly from an insurance company in the individual insurance market were turned down, were charged more, or had a specific health problem excluded from their coverage.1 Another survey found that 54 percent of people with individual market insurance were worried that their insurer would drop their coverage if they got really sick.2
Yet, the need for individual market coverage has increased as job-based insurance has decreased. From 2007 to 2009, five million Americans lost employer-sponsored health insurance; the percentage of non-elderly Americans with employer-sponsored insurance dropped from 68 percent in 2000 to 59 percent in 2009.3 The percentage of small businesses that offer coverage to their employees dropped from 68 percent in 2001 to 59 percent in 2009 – although rose in 2010, in part, due to the Affordable Care Act’s small business tax credits.4 Despite the growth in the number of people without employer-sponsored insurance, coverage in the individual market has remained at about 5 percent of non-elderly Americans – and declined according to another survey. This is likely due to the increasing unaffordability and unattractiveness of individual insurance products, and to insurers’ increasing success in screening out applicants with pre-existing conditions.5
With the declines in employer-sponsored coverage and individual market coverage, the number of non-elderly uninsured climbed to 50 million in 2009 – nearly one in five non-elderly Americans. The growing number of uninsured, particularly those with pre-existing conditions, has both health and cost consequences. About 60 percent of the uninsured who have chronic conditions delayed care and did not fill a prescription due to cost.6 Lack of coverage often leads to medical debt, and uncompensated and expensive care in sites like emergency rooms, creating “hidden costs” in the system as people with insurance often end up paying higher rates to offset the cost of this care.
One in Two Americans Has a Pre-Existing Condition
This new analysis sheds light on the number of Americans gaining protections from discrimination based on pre-existing conditions under the Affordable Care Act. Because pre-existing conditions are determined by insurer practices which vary, two estimates of the number of non-elderly individuals likely to be denied coverage in the individual market were constructed. The first includes only conditions that were identified using eligibility guidelines from State-run high-risk pools that pre-dated the Affordable Care Act. These programs generally insure individuals who are rejected by private insurers. As such, the “lower bound” estimates are people with a health problem likely to lead to a denial or significant mark-up or carve-out of benefits. The second includes additional common health and mental health conditions (e.g., arthritis, asthma, high cholesterol, hypertension, and obesity) that would result in an automatic denial of coverage, exclusion of the condition, or higher premiums according to major health insurers’ underwriting guidelines identified using internet searches. Individuals with these conditions would at least get charged a higher premium but could also have benefits carved out or be denied coverage altogether. Both estimates are based on the most recent data available for 2008 (for a full description, see the Methodology section).
Between 50 and 129 million non-elderly Americans have at least one pre-existing condition that would threaten their access to health care and health insurance without the protections of the Affordable Care Act. This represents 19 to 50 percent of non-elderly Americans. To put this into perspective, the percentage of the U.S. population gaining protections under the Affordable Care Act is roughly 1.5 to three times the total number of elderly Americans.
These estimates represent a “snapshot” or profile of individuals at a particular point in time. An analysis of a survey that follows people over time found that, among healthy people – reporting very good or excellent health with no chronic conditions – today, 15 to 30 percent (depending on their age) will develop a pre-existing condition within the next eight years.7 Other studies have looked at individuals’ lifetime risk of developing particular illnesses. For example, the odds are that one in three women and one in two men will develop some type of cancer over the course of their life.8 Americans have roughly the same odds of developing coronary heart disease.9 With diabetes growing in prevalence, men have a one in three chance, women have a two in five chance, and Hispanic women have a one in two risk of developing diabetes.10 Stated simply, most people develop health problems over the course of their lifetime that can be helped by health care, making access to such health care critical.
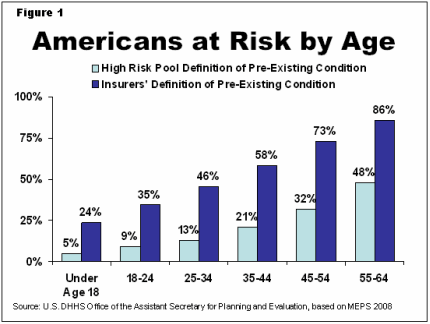
Up to 86 Percent of Older Americans Have a Pre-Existing Condition
Not surprisingly, as people age, their likelihood of having – or having had – a health condition increases. Looking only at pre-existing conditions used in determining eligibility for high-risk pools, the percentage of Americans with these health conditions ranges from 5 percent of children to 48 percent of people ages 55 to 64. Adding in common conditions that major insurers generally use in medical underwriting raises the risk to 24 percent for children, increasing to 86 percent for people ages 55 to 64 (see Figure 1).
Translating these percentages into numbers of people, there are 4 to 17 million children under age 18 with some type of pre-existing condition. Already, due to the new health reform law, insurers cannot deny coverage to children under the age of 19 based on a pre-existing condition – a protection that would be revoked without the health reform law.
A Higher Proportion of People with Employer-Sponsored Insurance Have Health Issues
The percentage of people with pre-existing conditions varies by insurance status – with the highest rates among those with employer-sponsored insurance, ranging from 21 to 54 percent (see Figure 2). Generally, pre-existing conditions matter less for people insured through employers that have a large risk pool and can therefore spread the cost of workers’ illnesses or injuries. In addition, some insurance protections already exist for people changing jobs.
However, 32 to 82 million people with both health problems and job-based coverage would be vulnerable without the new law. Increasingly, employers have used annual and lifetime limits on benefits to keep their health insurance costs down. In 2009, roughly 94 million Americans were in employer-sponsored insurance with a lifetime limit.11 The new health reform law has already banned lifetime limits in private insurance and has restricted annual limits for group and new individual market plans before banning such limits in 2014. This protects workers and their dependents with health conditions, whose coverage may have otherwise run out with a serious accident, disease that involves intense care, or other high-cost illness.
In addition, workers with a pre-existing condition may be less able to change jobs for fear of losing that coverage. Chronically ill workers are 40 percent less likely to leave their job if they get insurance through it compared to those that get insurance elsewhere.12 This “job lock” is common: individuals and families often make job and career decisions based on protecting insurance for themselves or a member of their family who may not otherwise have health insurance. This is especially true among older workers, the majority of whom have a pre-existing condition. Such workers may want to take early retirement, reduce their hours to part-time work, or go into business on their own, but that is often not possible given the likely loss of employer-based and non-underwritten health insurance. There are similar issues with changes in family status: getting divorced or aging out of eligibility for dependent coverage, for example, could also limit insurance access for people with pre-existing conditions in a system without the protections of the Affordable Care Act.
People who work in small businesses, along with their employers, may be discriminated against by their insurers due to a pre-existing condition. About 25 percent of people with employer-based coverage are in small group policies.13 In most States, insurers can engage in “experience rating,” or take into account the cost of workers or family members with pre-existing conditions within the employer group. As such, workers’ rates may spike with one worker’s illness or injury. In addition, small businesses are susceptible to having to scale back or drop coverage when they hire a worker with a pre-existing condition, or when one of their workers gets sick. Small businesses pay on average 18 percent more than large businesses for comparable coverage, in part due to the challenges of covering people with pre-existing conditions.14
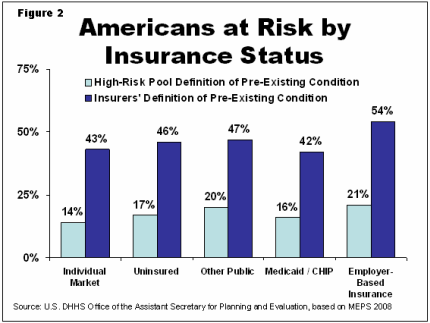
Fewer People with Individual Market Coverage Have Health Issues
Given insurers’ incentives to exclude people with pre-existing conditions from individual insurance in most States, it is not surprising the proportion of enrollees with health issues in this market tends to be lower than that in other markets. We estimate that 14 to 43 percent of enrollees in the individual market have a pre-existing condition – one-third to one-fifth less than the prevalence of pre-existing conditions among those with employer-sponsored insurance. This is consistent information from the industry; one insurer, for example, reported that nearly 15 percent of its enrollees in 2010 had a “rider” that limited covered or increased deductibles for certain medical conditions.15
Currently, there is very little coverage of children with pre-existing conditions in the individual market –1 to 8 percent of children enrolled in this type of coverage has a pre-existing condition, accounting for at most 140,000 out of a total of 1.9 million children enrolled in this market. In part, this results because Medicaid and the Children’s Health Insurance Program (CHIP) help low-income and sick children get needed health care. However, despite coverage offered by Medicaid and CHIP, up to 2 million children with pre-existing conditions are uninsured. The new health law prohibits insurers from denying coverage to children based on a pre-existing condition.
Nearly One in Five Americans with a Pre-Existing Condition Is Uninsured
The number of people who both have a pre-existing condition and are uninsured ranges from 9 to 25 million – or as much as 46 percent of the uninsured. Among non-elderly people with some type of pre-existing condition, about one in five, or 19 percent, is uninsured. Although the lack of affordable coverage remains the primary reason why Americans are uninsured, getting rid of discrimination against people with pre-existing conditions is critical to the success of the tax credits and State-based Exchanges that take effect in 2014.
Health Reform Ends Discrimination Based on Pre-Existing Conditions – Without It, Insurers Would Be Back in Charge
A central element of the Affordable Care Act, passed by the last Congress and signed into law by the President, is a new set of patient protections that prohibit insurance companies from denying coverage to Americans because they need it. Starting in 2014:
- Insurers can no longer use health status to determine eligibility, benefits, or premiums;
- Individuals and small businesses can choose from a range of private insurance plans through competitive marketplaces called Exchanges in their States; and
- Annual dollar limits on coverage will be banned in group and new individual market plans, critical benefits will be covered, and out-of-pocket spending will be limited.
These new protections add to a strong set that have already been put in place to increase access to health care coverage for Americans with pre-existing conditions such as:
- Insurers can no longer limit lifetime coverage to a fixed dollar amount;
- Insurers can no longer take away your coverage because of a mistake on an application;
- Insurers can no longer deny coverage to a child because of a pre-existing condition;
- Thousands of uninsured people with pre-existing conditions have enrolled in the temporary high-risk pool program called the Pre-existing Condition Insurance Plan, which has literally saved people’s lives by covering services like chemotherapy.
Rescinding the new health insurance protections would, now and starting in 2014:
- Reduce the health care and health insurance options of the 50 to 129 million Americans with pre-existing conditions;
- Take away, for the 32 to 82 million people with both a pre-existing condition and job-based insurance, the ban on lifetime limits on benefits, restrictions on annual limits on benefits, new protections in the small group market from discrimination based on health status, and the security of knowing you can change jobs without losing your health coverage and care;
- Lock older Americans into their current coverage if they have it, since up to 86 percent of people ages 55 to 64 have some type of pre-existing condition;
- Limit insurance options for the parents of the up to 2 million uninsured children with pre-existing conditions, who today can no longer be blocked from purchasing individual market insurance due to their pre-existing condition.
Methodology
The U.S. Department of Health and Human Services’ Office of the Assistant Secretary for Planning and Evaluation (ASPE) produced this analysis. The 2008 Medical Expenditure Panel Survey (MEPS) was used to identify individuals who would likely be denied due to a pre-existing condition if they were to apply for coverage in the individual market. A multi-pronged approach was used to identify conditions that would certainly or likely exclude individuals from being offered coverage. This condition list was generated from two sources: eligibility guidelines from 19 pre-Affordable Care Act high-risk pools and underwriting guidelines from seven major insurance carriers.16 The MEPS was used to identify whether individuals had a medical visit for any of these conditions, experienced any disability days as a result of any of these conditions, and reported that they were bothered by any of these conditions in the past year. Additional questions regarding whether individuals had ever been diagnosed with a smaller set of conditions from these lists were used to further refine our measure.
Two estimates of the share of non-elderly individuals likely to be denied coverage in the non-group market are presented. The first includes only conditions that were identified using eligibility guidelines from high-risk pools; and the second includes five additional common conditions (arthritis, asthma, high cholesterol, hypertension, and obesity) and a number of common mental health conditions that would result in an automatic decline, exclusion of the condition, or higher premiums according to the seven insurer guidelines examined. The first estimate includes conditions that will very likely cause an applicant to be denied coverage, and should be considered a lower bound estimate. The second estimate includes conditions that might result in a denial of coverage, but also might result in a “rate-up” (that is, a higher premium) or a coverage rider (that is, a policy that excludes coverage for a pre-existing condition). The following describes in more detail the methodology.
First Measure: High-Risk Pool Definition of Pre-Existing Conditions
Individuals likely to be uninsurable were identified in the following manner. An approach developed by the Lewin Group was replicated and identified conditions reported by five or more of the 19 pre-Affordable Care Act state high-risk pools as indicating automatic eligibility for enrollment in the pool.17 This list included the following conditions: alcohol and drug abuse, chemical dependency, acquired immune deficiency syndrome (AIDS), Alzheimer’s disease, angina pectoris, anorexia nervosa, aortic aneurysm, aplastic anemia, arteriosclerosis, artificial heart valve or heart valve replacement, ascites, brain tumor, cancer (excluding skin), cancer (metastatic), cardiomyopathy/primary cardiomyopathy, cerebral palsy/palsy, chronic obstructive pulmonary disease (COPD), chronic pancreatitis, cirrhosis of the liver, congestive heart failure, coronary artery disease, coronary insufficiency, coronary occlusion, Crohn’s disease, cystic fibrosis, dermatomyositis, diabetes, emphysema/pulmonary emphysema, Friedreichs’s disease/ataxia, hemophilia, active and chronic hepatitis, HIV positive, Hodgkin’s disease, hydrocephalus, intermittent claudication, kidney failure, kidney disease, and kidney disease with dialysis, lead poisoning with cerebral involvement, leukemia, Lou Gehrig’s Disease/amyotophic lateral sclerosis (ALS), lupus erythematosus, disseminate, and lupus, malignant tumors, major organ transplant, motor or sensory aphasia, multiple or disseminated sclerosis, muscular atrophy or dystrophy, myasthenia gravis, myocardial infarction, myotonia, paraplegia or quadriplegia, Parkinson’s disease, peripheral arteriosclerosis, polyarteritis, polycystic kidney, postero-lateral sclerosis, psychotic disorders, silicosis, splenic anemia, True Banti’s syndrome, Banti’s disease, rheumatoid arthritis, sickle cell anemia and disease, Stills disease, stroke, syringomyelia (spina bifida or myelomeningocele), tabes dorsailis, thalassemia (Cooley’s or Mediterranean anemia), ulcerative colitis and Wilson’s disease.18
Individuals were also identified who reported that they had “ever been diagnosed” with the following conditions: coronary heart disease, myocardial infarction, other heart disease, angina pectoris, stroke, emphysema, cancer, and diabetes.
Individuals who were identified by one of these mechanisms were considered unlikely to be insurable in the private non-group market and are the basis of the first estimate. This estimate should be considered a lower bound, as there are potentially more conditions that insurers consider an automatic decline of coverage.
Second Measure: Insurers’ Definition of Pre-Existing Conditions
To construct the second measure, we included additional conditions that are likely to cause an applicant to be denied coverage, be “rated up” (that is, charged a higher premium), or to be sold coverage with a rider that excludes coverage for one or more pre-existing conditions.
Individuals with five common conditions – arthritis, asthma, high cholesterol, hypertension, and obesity (BMI > 35) – were included in the second measure, as were individuals who had “ever been” diagnosed with arthritis, asthma, high cholesterol, or hypertension. These conditions were found to result in a denial, an exclusion of coverage for that condition, or a higher premium for individuals in all but one of the seven underwriting guidelines we examined.
In addition, individuals who were currently being treated for neurotic and related disorders, stress and adjustment disorders; conduct disorders; emotional disturbances; and including attention deficit hyperactivity disorder (ADHD) were included in the second measure, as were individuals who had ever been diagnosed with ADHD. These types of mental health conditions were identified in the underwriting guidelines as conditions that would result in denial, waiting periods, condition exclusions or higher premiums. Information from ASPE-conducted interviews with insurance commissioners indicated that individuals in treatment for mental health conditions were generally denied coverage in the individual market. Given the conflicting evidence, a conservative approach was used and these conditions were included in the second and not the first measure. Had these conditions been included in the first measure, the estimate of likely to be uninsurable individuals would have increased from 19 percent to 29 percent.
1 Doty MM, Collins SR, Nicholson JL et al. Failure to Protect: Why the Individual Insurance Market is not a Viable Option for Most US Families. The Commonwealth Fund, July 2009.
2 Kaiser Family Foundation. Survey of People who Purchase Their Own Insurance. June 2010.
3 Holahan J. “The 2007-09 Recession and Health Insurance Coverage,” Health Affairs, 30(1): 145-152, January 2011.
4 Levey NN, “More Small Businesses are Offering Health Benefits to Workers,” The Los Angeles Times, December 27, 2010.
5 Waxman HA; Stupak B. Memorandum: Coverage Denials for Pre-Existing Conditions in the Individual Health Insurance Market, October 12, 2010. Washington, DC: U.S. House of Representatives, Committee on Energy and Commerce.
6 Tu HT, Cohen GR. Financial and Health Burdens of Chronic Conditions Grow. Washington: Center for Studying Health System Change, April 2009.
7 Special Tabulations from the Panel Study of Income Dynamics (PSID) – years 1999, 2001, 2003, 2005 and 2007. Sample of adults drawn from the 1999 wave of the PSID and followed in subsequent waves over an eight year period to determine self report of the onset of any new conditions including stroke, high blood pressure, diabetes, cancer, chronic lung disease, heart attack, coronary heart disease, emotional, nervous, or psychiatric problem, arthritis, asthma, and permanent loss of memory.
8 National Cancer Institute, SEER Cancer Statistics Review, 2007-2009. July 2010; http://seer.cancer.gov/csr/1975_2007/results_merged/topic_lifetime_risk_diagnosis.pdf
9 National Heart, Blood and Lung Institute, http://www.nhlbi.nih.gov/new/press/hlb07-99.htm
10 Centers for Disease Control and Prevention. “CDC Statements on Diabetes Issues: Lifetime Risk for Diabetes Mellitus in the United States,” http://www.cdc.gov/diabetes/news/docs/lifetime.htm
11 See the regulatory impact analysis in the interim final regulation implementing the lifetime limit policy, 75 Federal Register 37188, June 28, 2010.
12 Stroupe KT, Kinney ED, Kniesner TJJ. “Chronic Illness and Health Insurance-Related Job Lock,” Journal of Policy Analysis and Management, 20(3): 525-544, Summer 2001.
13 See the regulatory impact analysis in the interim final regulation implementing the preventive services policy, 75 Federal Register 41726, July 19, 2010.
14 Gabel J et al. “Generosity and Adjusted Premiums in Job-Based Insurance: Hawaii is Up, Wyoming is Down,” Health Affairs, 25(3): 832-843, 2006.
15 Waxman HA; Stupak B. Memorandum: Coverage Denials for Pre-Existing Conditions in the Individual Health Insurance Market, October 12, 2010. Washington, DC: U.S. House of Representatives, Committee on Energy and Commerce.
16 Underwriting guideline used include: Aetna Inc., Aetna Advantage Plans for Individuals and Families, Underwriting Guidelines., 2010, pp. 10-23. Blue Cross of California, CaliforniaAgent Guide, Oct., 2010, pp 36-58.; Blue Shield of California, Application and Underwriting Process Guide. Aug., 2008, pp. 21-42. ; Health Net Inc., Field Underwriting and Enrollment Guidelines, Jan., 2006, pp. 11-20. On the internet at: http://binsuredhere.com/health_net.htm; Vista Healthplan and its affiliate, VISTA South Florida, Individual Product Agent Guide. 9/2006. UnitedHealthcare, Golden Rule Insurance, Underwriting Guidelines, Aug., 2009, pp. 25-30.
HumanaOne Health and Life Products, Agent Eligibility and Underwriting Guide 2009-2010.
17 Families USA Foundation. Health Reform: Help for American with Pre-Existing Conditions. May 2010.
18 The Lewin Group analysis also included obesity (BMI > 35) on the list of conditions that would cause a denial. We did not find obesity on the condition lists used by state high-risk pools, and therefore did not include it in the list of conditions that would almost certainly lead to a denial.